Conditions Treated
Base of Thumb Arthritis
What is it?
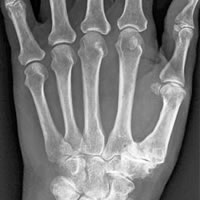
The joint at the base of the thumb (Carpometacarpal or CMC joint) is made up of 2 bones, the thumb metacarpal and the trapezium. It is a saddle shaped joint and very mobile, allowing movement of the thumb in many directions. Because it is so mobile and is used a huge amount it is prone to" wear and tear" or osteoarthritis, destroying the smooth cartilage of the joints; this results in painful bare bone grinding on bare bone.
What causes it?
Osteoarthritis or "wear and tear" is related to age, use and trauma. It commonly affects females over 40 years old and may be present in both thumbs.
What are the symptoms?
Patients commonly present with a dull ache in the base of the thumb that is severely exacerbated by use, most commonly activities such as wringing out a cloth or opening jars and bottles; this severe pain is often described and "grinding".
With time the thumb base may become more pronounced or "shouldered" as the joint destruction progresses and the joint subluxes. Patients may find that the range of movement in the thumb is diminished, as is their grip strength.
Do I need any further investigations?
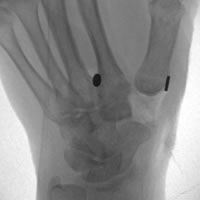
YES. All patients require x-rays of the thumb base and surrounding joints to assess the degree of arthritic change and allow for pre-operative planning.
What is the treatment?
Early arthritic changes often respond very well to activity modification and avoidance in combination with splinting from your hand therapist.
Cases that don't respond to this non-operative treatment and more severe case are then treated with an injection of steroid and local anaesthetic, which is performed under x-ray guidance to insure correct placement. This procedure is partly diagnostic and partly therapeutic. If the pain improves at all, then one can be confident that the diagnosis is correct. Many people find that the pain worsens for a week or so after the injection and then improves.
Cases that are resistant to the above treatment may well require surgical intervention. There are several options depending on the severity of the disease, age and requirements of the patient.
- Trapeziumectomy and Mini Tightrope Stabilization.
Trapeziumectomy is a well-established and recognized treatment for this problem. The operation involves removing the arthritic trapezium do that it no longer grinds against the base of the thumb. To prevent the thumb " falling back" into the hand, Andy uses a new technique that involves suspending the thumb to the index finger using a very string stitch. This is the mainstay of treatment for CMC joint arthritis in Andys' practice. - Joint replacement
Whilst it is possible to replace the CMC joint, there is no evidence that patients do any better than if they have a simple trapeziumectomy. The operation to replace the joint is much more complex and carries a higher risk of complications. As such, Andys' indications for this operation are very limited. This is something he will discuss with you at your consultation. - Joint Fusion
Fusion of arthritic joints reliably relieves pain but at the sacrifice of movement. Fusion operations around the thumb are difficult and carry a higher risk of complication than simple trapeziumectomy. Andy generally reserves fusion of the joint for young manual workers.
How long will it take to recover?
In general recovery following any of the operations above takes 6 weeks. Following the operation your thumb and wrist will be in a temporary plaster. You will be seen by a hand therapist at 2 days who will get you moving your hand very early after surgery to avoid stiffness.
The stiches are removed at around 10 days and Andy will review you at that point.
If you have had a trapeziumectomy or replacement you will be fitted with a custom made plastic splint by your hand therapist. This will give you some support but will allow you to get the thumb moving. Following your 2 week appointment your hand therapist will get you moving your hand more and more and will also advise how to help soften and desensitize the scars.
If you have had a fusion, you will spend another 4 weeks in a full, lightweight thumb cast.
Most patients have discomfort following the operation but this is different from the original pain prior to the operation. It takes 3-6 months for patients to feel the full benefit of these procedures.
What are the potential complications?
- Infection - Uncommon and usually treated very successfully with antibiotics
- Delayed healing - Smokers and those with diabetes are more prone to this
- Painful/Tender Scars - the vast majority of patients complain of some discomfort around the scar and thumb, this is know as pillar pain and generally resolves with time. Rigorous wound care and desensitization as directed by your hand therapist help prevent this.
- Damage to surrounding structures - inadvertent damage or stretching to surrounding nerves may cause some numbness around the scars, although this should improve with time.
- Stiffness - Operations to the hand may cause stiffness, this can be minimized by working closely with your hand therapist and getting your hand moving as early as possible.
- CRPS - An uncommon but potentially serious complication of hand surgery leading to pain, swelling and discomfort. It is impossible to predict this problem but working closely with you hand therapist and getting your hand moving early has been proven to significantly reduce the risk of this.
When can I get back to normal activities?
The hand MUST be kept clean and dry for 10 days until the sutures are removed. Depending the site and extent of your surgery you should be able to return to "desk job" type activities within 3-4weeks of the operation. Any manual work, heavy lifting or sporting activities should be avoided for at least 6-8 weeks.
You may return to driving in around 4-6 weeks. Please inform your insurance company that you have recent hand surgery to ensure that are happy for you to do so.