Conditions Treated
Dupuytren's Disease
What is it?
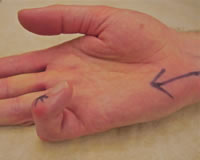
Dupuytren's Disease is named after a French anatomist and military surgeon Baron Guillaume Dupuytren(1777-1835) It is a common condition caused by the abnormal thickening of a layer of tissue within the hand and fingers. This thickening causes lumps and cords of tissue to develop in the skin of the hand; as this tissue matures, it contracts causing the fingers to curl into the palm. These deformities make using the hand for everyday activities such as washing your hair, shaking hands or putting gloves on, very difficult.
What causes it?
Dupuytren's disease has a strong genetic component and it is likely that somebody in your family may have been affected by it at some point. It occurs more commonly in men over the age of 40 and is thought to have been bought to the UK by the Vikings.
The little and ring fingers are most commonly affected and people with diabetes, lung disease, high alcohol intake, smokers and those on certain medications are at higher risk.
What are the symptoms?
People generally come to me when they find they are not able to use their hands for normal daily activities such as washing their hair or putting their hand in their pocket. This is because the fingers are curled into the palm of the hand and "get in the way". Some patients may also find that they develop pits or deep creases in the hand that they find very difficult to keep clean and dry, others may have painful, thickened skin or nodules in the hand
Do I need any further investigations?
No. Dupuytren's disease is a clinical diagnosis and no further investigations would be required as long as this was your only symptom.
What is the treatment?
As the disease is genetic, it is "part of you". Treatment addresses the diseased tissue that is in the hand and fingers at the time of surgery but does not eradicate the underlying disorder, thus there is a chance that the deformities may recur or worsen with time, even after treatment.
The type of treatment depends on the extent and severity of the disease, which finger joints are affected and your general health and well-being.
The majority of these procedures are carried out under a general anaesthetic as a day case, although some may be carried out under local anaesthetic or regional block.
- Percutaneous Fasciotomy/ Needle Aponeurectomy
This minimally invasive procedure is performed under local anaeasthetic in patients with very well defined cords of disease in the palm. A needle or small blade is used to weaken the cords, allowing the fingers to be straightened. As the tissue isn't removed the rate of recurrence is higher than other forms of treatment, however the recovery period is much shorter and less complicated. - Open Fasciectomy
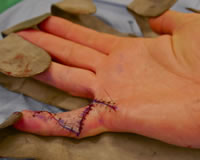
This is the mainstay of treatment for Dupuytren's disease in Andy's practice. It involves removing the diseased tissue from the hand and fingers through a series of zigzag incisions. This procedure allows for better straightening of the fingers, especially in long standing cases of deformity. The recurrence rate is much lower than other less invasive treatments but has a longer recover time. - Dermofasciectomy
Reserved for cases that have had previous surgical treatment, dermofasciectomy involves taking a skin graft from the wrist or forearm to replace the scarred and diseased skin in the palm and fingers. The recovery time for this is longer than other treatments - Ziapex™ Injection
A new invention that uses an enzyme that is injected into the cords of the palm and fingers; this dissolves the collagen in the tissue, which provides it's with its strength. After a few days the fingers are then straightened under local anaestehtic. As the diseased tissue is not removed, the rate of recurrence is higher than an open procedure. This is a relatively new treatment that has only been used in the UK for 1 year.
How long will it take to recover?
Recovery depends on the type of surgery that you have. In general following an open fasciectomy, the hand will be put into a temparory plaster splint and a sling to allow for swelling and postoperative discomfort to settle. You will be seen by a hand therapist at 2 days who will remove this, clean and redress the wounds for you. At this point a custom plastic splint maybe be made for you to wear, this will be dependent on the severity of the deformity. The hand therapist will get you moving your hand very early after surgery to avoid stiffness.
The stiches are removed at around 10 days and Andy will review you at 2 weeks.
Following your 2 week appointment your hand therapist will get you moving your hand more and more and will also advise how to help soften and desensitize the scars.
What are the potential complications?
Any surgical procedure carries risks, however every effort is made to minimize these to ensure the best possible outcome from your surgery.
- Infection - Uncommon and usually treated very successfully with antibiotics
- Delayed healing - Smokers and those with diabetes are more prone to this
- Painful/Tender Scars - Rigorous wound care and desensitization as directed by your hand therapist help prevent this.
- Stiffness - Operations to the hand may cause stiffness, this can be minimized by working closely with your hand therapist and getting your hand moving as early as possible.
- CRPS - An uncommon but potentially serious complication of hand surgery leading to pain, swelling and discomfort. It is impossible to predict this problem but working closely with you hand therapist and getting your hand moving early has been proven to significantly reduce the risk of this.
- Recurrence - as the disease is "part of you" it may recur after surgical treatment. 30% at 5 years.
- Incomplete correction of deformity - sometimes it is impossible to fully straighten the fingers, especially if the deformity is severe or long standing.
- Damage to the digital nerve/artery - Occurs in less than 1% of patients and would require surgical repair. Despite this numbness of the finger may still persist.
When can I get back to normal activities?
The hand MUST be kept clean and dry for 2 weeks. Once the sutures are removed and you are moving your hand with the therapist you may commence gentle "Desk Job" type activities. Any manual work, heavy lifting or sporting activities should be avoided for at least 6 weeks. You may return to driving in 3-4 weeks depending on the extent of your surgery. Please inform your insurance company that you have recent hand surgery to ensure that are happy for you to do so.